India’s Resurgence of COVID-19: Urgent Actions Needed

Cover photo: Copyright © 2021 Reuters/Navesh Chitrakar
THE LANCET
12 June 2021
 The Lancet Citizen's Commission on Reimagining India's Health System has made eight recommendations to ramp up India's health services and to sustain the common man during a Covid-like pandemic. Regarding Lancet's recommendation five on centralised vaccine procurement, the Government of India has already taken care of it on Monday 7th June when Prime Minister Narendra Modi announced at 5 pm during his nationwise televised speech: “From June 21, the Government of India will provide free vaccines to all states for the 18-plus-year-old people.” He announced the central government would now directly buy 75 per cent of the vaccines from the manufacturers and give it to the states. The remaining 25 per cent, he said, would be left for private hospitals to buy directly from the manufacturers. This U-turn of the Central Government has much to do with the 75 (Central Govt) :25 (Private hospitals) formula advocated by Mr Uday Kotak – CII President and CMD of Kotak Mahindra Bank. Regarding the sixth recommendation on Community Engagement and Public Participation, NGOs have been playing a very vital role in this. To facilitate their role, the current stringent FCRA account norms for NGOs (especially those with proven record of social service) need a relook, in particular 20% ceiling on Administrative Cost. After all these NGOs are brining in overseas funds for the uplift of India from the grassroots level, something which the government is unable to do single-handedly.
The Lancet Citizen's Commission on Reimagining India's Health System has made eight recommendations to ramp up India's health services and to sustain the common man during a Covid-like pandemic. Regarding Lancet's recommendation five on centralised vaccine procurement, the Government of India has already taken care of it on Monday 7th June when Prime Minister Narendra Modi announced at 5 pm during his nationwise televised speech: “From June 21, the Government of India will provide free vaccines to all states for the 18-plus-year-old people.” He announced the central government would now directly buy 75 per cent of the vaccines from the manufacturers and give it to the states. The remaining 25 per cent, he said, would be left for private hospitals to buy directly from the manufacturers. This U-turn of the Central Government has much to do with the 75 (Central Govt) :25 (Private hospitals) formula advocated by Mr Uday Kotak – CII President and CMD of Kotak Mahindra Bank. Regarding the sixth recommendation on Community Engagement and Public Participation, NGOs have been playing a very vital role in this. To facilitate their role, the current stringent FCRA account norms for NGOs (especially those with proven record of social service) need a relook, in particular 20% ceiling on Administrative Cost. After all these NGOs are brining in overseas funds for the uplift of India from the grassroots level, something which the government is unable to do single-handedly.
According to Business Standard India 21 May 2021, India has so far administered 191,879,503 vaccine doses. Among Indian states, the top 5 in terms of number of vaccine shots administered are Maharashtra (25209030), Uttar Pradesh (20467359), Rajasthan (20462219), Gujarat (19130473), and West Bengal (17057029). As on today approximately 4% of India's population has been fully vaccinated.
India needs an estimated 250 million COVID-19 vaccine doses each month to equip vaccination drives to full capacity. But as of now it has only around 70–80 million doses per month. This means India has to ramp up its production facilities including import (not from China please!) by more than 300%. Nothing short of a miracle can help India achieve this target. India also has to meet its commitment to its neighbours, in particular Nepal, where Serum has so far supplied only 50% of its order book and could not supply the balance on account of a blanket ban on export of vaccines by the Government of India due to acute domestic shortage. This is the underlined raison d'être for increasing the Covishield gap between the first and second doses from 8 weeks to 12-16 weeks.
Let's hope the vaccine supply position improves considerably by July-August. It's high time the Central and State Governments (as Health is a state subject) woke up to the Lancet recommendations and worked together in a spirit of federalism, bearing in mind the importance of lives and livelihood. For seamless coordination of health services, Logistics and Supply Chain Management will be a key area. Isaac Gomes, Associate Editor, Church Citizens' Voice.
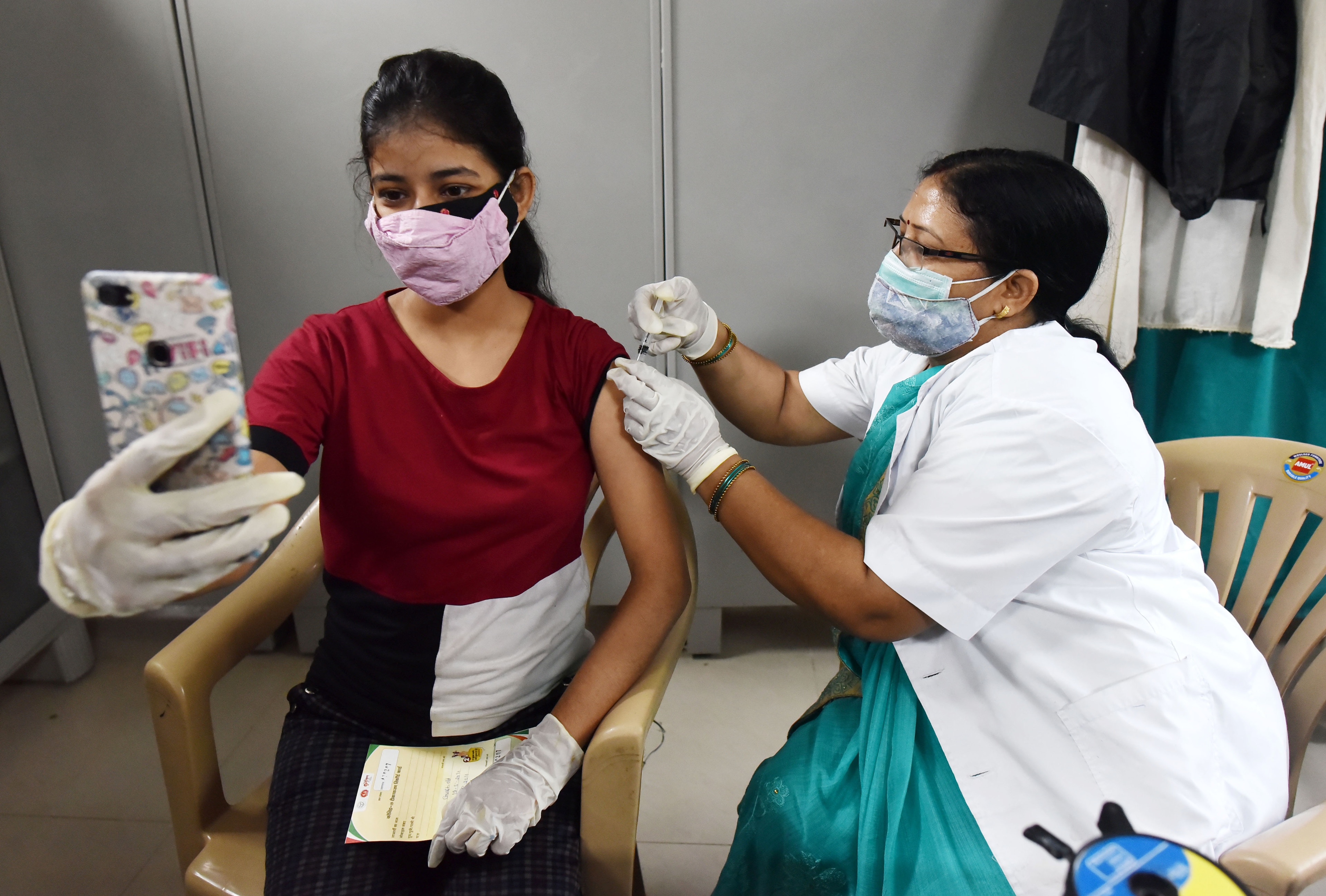
A medic administers the dose of vaccine to a beneficiary, at Moti Lal Nehru Medical College vaccination in Prayagraj on Thursday. (Business Standard 21.05.2021)
As of May, 2021, the resurgent wave of COVID-19 in India has been spreading to rural populations and other countries in the region. The pandemic has foregrounded the long-standing need for universal health coverage (UHC) in India. The Lancet Citizens' Commission on Reimagining India's Health System was launched in December, 2020, to map the pathway to achieving UHC in the coming decade through a participatory, solutions-driven approach.
Yet in the present moment, India confronts an immediate emergency to save lives and reduce suffering. On behalf of the Lancet Citizens' Commission, we propose eight recommendations for the central and state governments that share responsibility for the health of the India's people. Our recommendations complement those of Kuppalli and colleagues' call for actions from the international community.
Our intention in making these recommendations, some of which have been recently voiced by authoritative voices in the country, is to amplify and synthesise what must be done urgently.
First, the organisation of essential health services must be decentralised. A one-size-fits-all approach is untenable since the numbers of COVID-19 cases and health services differ substantially from district to district.
District-level working groups that have the autonomy to respond to rapidly changing local situations must be empowered to receive funds and resources to coordinate efforts across all sectors of the health system, from front-line workers to tertiary care. Appropriate technologies could have a role in streamlining the management of resources and supplies, such as hospital beds, oxygen, ambulances, and funeral resources. Several states and districts have successfully used such decentralised systems for quarantine, triage through front-line workers, and community-based primary service delivery.
Second, there must be a transparent national pricing policy and caps on the prices of all essential health services, for example, ambulances, oxygen, essential medicines, and hospital care. Hospital care should not require any out-of-pocket expenditure and costs should be covered by existing health insurance schemes for all people, as has been done in some states.
All local governments must be allocated their grants as recommended by the Fifteenth Finance Commission to ensure they have the resources to augment COVID-19-related health services in their jurisdictions.
Third, clear, evidence-based information on the management of COVID-19 must be more widely disseminated and implemented. This information should include suitably adapted international guidelines for home care and treatment, primary care, and district hospital care in local languages that incorporate local circumstances and clinical practice. The guidance must also emphasise what not to do and ensure that only evidence-based therapeutics are used. It should also provide information to help prevent increasingly concerning reports of other impacts of COVID-19, including secondary infections such as mucormycosis.
The information should also underline the essential non-COVID-19 health services that must remain fully accessible in specific facilities. For example for tuberculosis, maternal and child health, and emergency medicine. Specific guidance should be offered by the central government on the appropriate use of Indian systems of medicine, especially for prevention and health promotion interventions, such as yoga.
Additionally, widespread access to teleconsultation and care delivered by front-line workers needs to be expanded to reduce the burden on hospitals.
Fourth, all available human resources across all sectors of the health system, including the private sector, must be marshalled for the COVID-19 response and adequately resourced, particularly with sufficient personal protective equipment, guidance on the use of clinical interventions, insurance, and mental health support. We support the implementation of the decision to deploy final-year medical students and AYUSH (ayurveda, yoga, naturopathy, unani, siddha, and homoeopathy) students in the COVID-19 response; this policy should be extended to nursing and paramedical students.
Fifth, central systems to procure and distribute COVID-19 vaccines free of cost should be established in a departure from the current policy of decentralised procurement through state governments.
Such an approach would optimise prices and minimise cross-state inequities that may result from differential fiscal and capacity contexts. By May 19, 2021, only 3% of India's population was fully vaccinated; up to 250 million COVID-19 vaccine doses are estimated to be needed each month to equip vaccination drives to full capacity and the country only has around 70–80 million doses per month.
State governments must decide on the priority groups for vaccination on the basis of evidence to optimise the use of available vaccine doses, which can be incrementally expanded as supplies improve. Vaccination is a public good and should not be left to market mechanisms.
Sixth, community engagement and public participation must lie at the heart of India's COVID-19 response. Grassroots civil society has historically had a crucial role in people's participation in health care and other development activities, such as in strengthening the COVID-19 response in Mumbai.
We recommend active collaboration between government and civil society organisations to create and disseminate accurate information, enabling home-based care, emphasising prevention, helping navigate access to live-saving treatment, and promoting vaccination. Restrictions on the capacity of non-governmental organisations to access foreign or domestic corporate social responsibility financial resources and human resource support must be immediately withdrawn.
Seventh, there must be transparency in government data collection and modelling to enable districts to proactively prepare for the likely caseloads in the coming weeks. Health system personnel require data on age and sex disaggregated COVID-19 cases, hospitalisations, and mortality rates; community-level coverage of vaccination; and community-based tracking of the effectiveness of COVID-19 treatment protocols and long-term outcomes. Additionally, surveillance needs to include urgent investment in genomic sequencing, adequate institutional capacity, and trained personnel to provide real-time alerts of SARS-CoV-2 variants, hot spots, and breakthrough infections.
Finally, the profound suffering and risk to health caused by loss of livelihoods should be minimised by making provisions for cash transfers by the state to workers in India's vast informal economy who have lost their jobs, as is being done by some state governments.
Formal sector employers must be required to retain all workers, irrespective of the status of contracts, through a government commitment to offer compensation to these companies when the economy revives. If lockdowns are deemed necessary, on the basis of local epidemiological data, they must be announced well in advance and entail planning for all essential services.
















